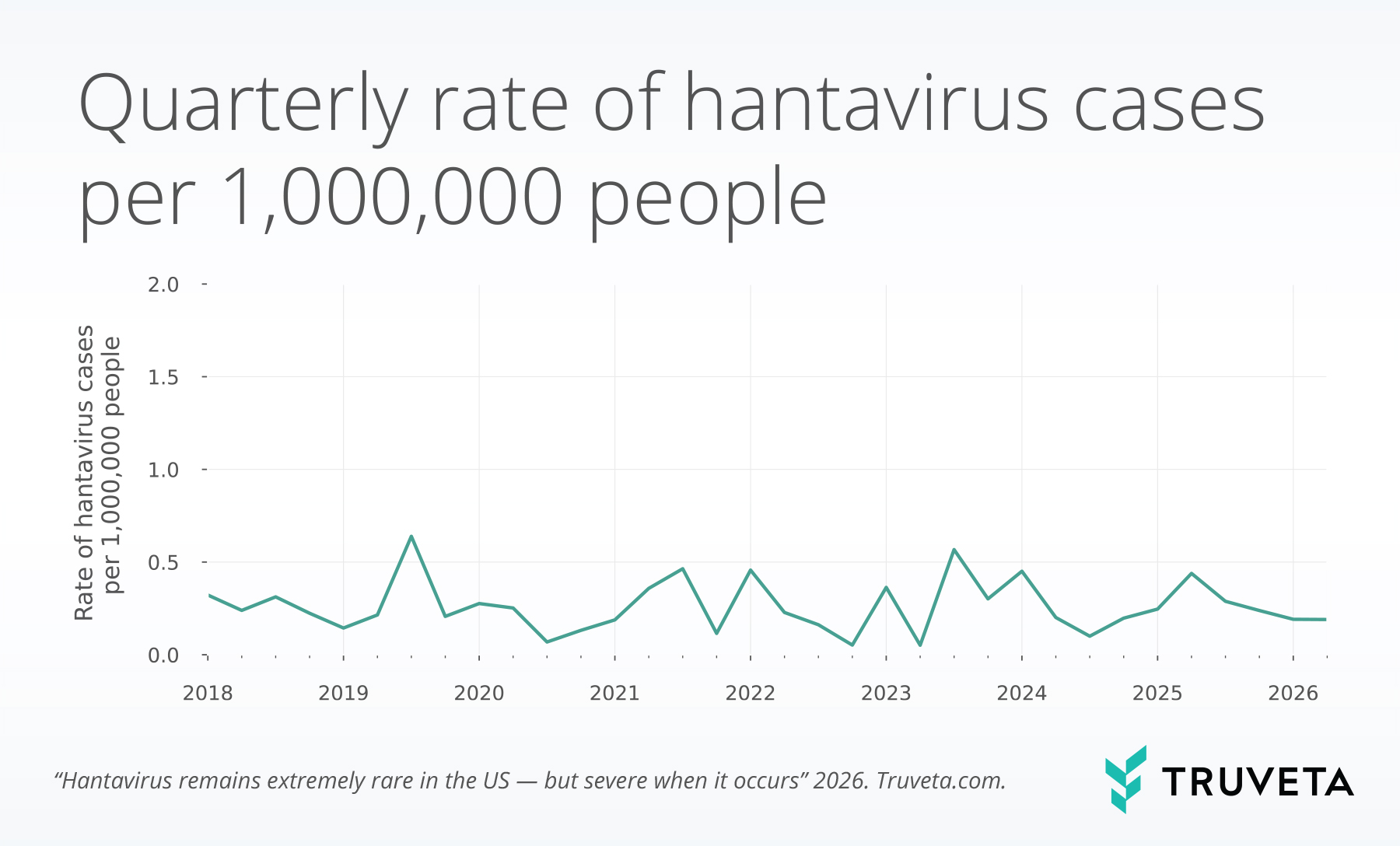
- Since 2018, roughly 0.3 hantavirus cases per 1 million patients seeking care each quarter were identified.
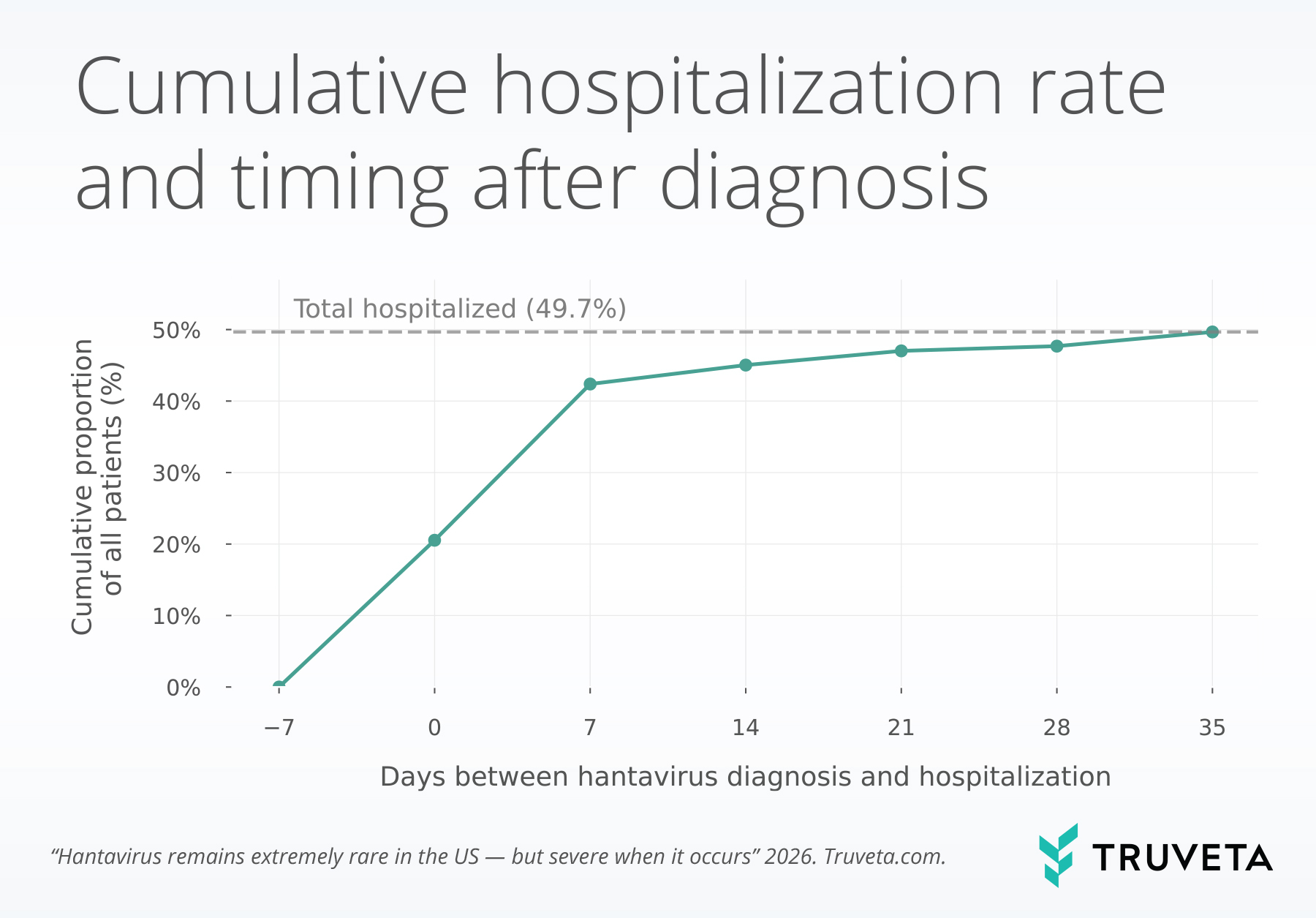
- Nearly half of patients with hantavirus were hospitalized within first 14 days. Of patients who were hospitalized, 85% were hospitalized prior to diagnosis or within the first week of their diagnosis.
Hantavirus is a rare but potentially life-threatening viral infection primarily spread through exposure to infected rodent urine, droppings, or saliva (1). In the United States, hantavirus infections are most commonly associated with deer mice; however, in rare cases the Andes variant of hantavirus has been shown to spread person-to-person, when they are in close contact (2, 3). Hantavirus infections damage the lining of small blood vessels, causing vascular leakage throughout the body. The disease can manifest along a spectrum, but is generally described based on whether the lungs or kidneys are predominantly affected (4, 5). Although infections are uncommon, hantavirus has a high reported mortality rate and often requires intensive medical care once severe symptoms develop (1, 6). Currently, there is no antiviral treatment approved for hantavirus infection, and management is largely supportive, emphasizing the importance of early recognition and hospitalization when severe disease occurs (6, 7).
On May 2, 2026, a hantavirus outbreak was reported on a cruise ship in the Atlantic Ocean. To date, three individuals who were on the ship have died and more have tested positive (8, 9). This outbreak has spurred renewed public health alerts and interest in understanding the real-world clinical burden of disease among patients with hantavirus. However, because hantavirus is rare, data describing complications and healthcare utilization remain limited. Real-time electronic health record (EHR) data can provide insight into the complications observed among patients diagnosed in routine clinical practice.
Using a subset of Truveta Data, we examined patients with a documented hantavirus diagnosis since 2018 to better understand complications and healthcare utilization following diagnosis.
Methods
Using a subset of Truveta Data, we identified patients with evidence of a hantavirus diagnosis between January 2018 and April 2026. We report the quarterly percentage of patients diagnosed with hantavirus among all patients with any recorded diagnosis. This normalization approach provides context for temporal trends by accounting for fluctuations in the number of patients seeking care each quarter.
We also evaluated hospitalizations occurring 7 days prior to and 35 days following the hantavirus diagnosis. We describe trends in diagnosis timing.
Results
We identified 151 patients with a hantavirus diagnosis since 2018. Most patients were over the age of 45 (66.8%), male (50.3%), White (70.9%), and not Hispanic or Latino (72.2%). Hantavirus cases remain extremely rare—on average, there are 0.3 cases per 1,000,000 people with a diagnosis each quarter.
Hospitalizations
Patients with hantavirus were commonly hospitalized. Approximately 1 in 2 patients with hantavirus were hospitalized within the 7 days prior to diagnosis or within the 35 days after diagnosis. Of the patients who were hospitalized, 85.3% were hospitalized within the first week of diagnosis.
Discussion
In this real-world analysis of patients with hantavirus, we observed hantavirus cases have remained rare since 2018. We also observed high rates of hospitalizations. Nearly half of patients had evidence of hospitalization within 30 days. These findings are consistent with the known clinical severity of hantavirus infections and reinforce the substantial healthcare burden associated with this condition (5, 7, 10). However, current evidence on hantavirus remains largely limited to case reports, which provide rich clinical detail but may not capture broader patterns of hospitalizations and outcomes across health systems. This descriptive analysis using large-scale EHR data is intended to provide an earlier characterization of hospitalizations.
During an outbreak, the questions clinicians and health systems need answered arise faster than evidence can be generated. The return of some individuals aboard the MV Hondius cruise ship to Nebraska on May 11, 2026 highlights how quickly health systems may need to prepare for the possibility of severe disease requiring hospitalization. While public health systems and officials are currently monitoring these exposed individuals and limiting transmission, clinicians also need early information about potential complications and patterns of care among patients with hantavirus.
Although cases associated with the MV Hondius are not included in this analysis, these findings demonstrate how existing EHR data infrastructure can support near real-time assessment of clinical outcomes during emerging outbreaks. Given increasing public awareness during recent outbreaks and the absence of targeted antiviral therapies for hantavirus, understanding the downstream complications associated with the disease and tracking new cases remain important for clinicians and public health officials.
These findings should also be interpreted in the context of known under-diagnosis of hantavirus infections. Prior studies suggest that many infections are never clinically identified. For example, studies from Finland estimate that only approximately 15% of hantavirus infections are diagnosed and reported (10, 11). This analysis reflects patients who sought medical care because of clinically significant illness or complications. Second, we used diagnostic codes to identify patients rather than laboratory-confirmed infections. Laboratory confirmation improves diagnostic specificity and helps distinguish acute hantavirus infection from other illnesses with similar clinical presentations. Additionally, hospitalizations for patients who sought medical care at a different health system after diagnosis may not be captured in the hospitalization rates analysis.
Despite these limitations, this study demonstrates how EHR data can provide timely insight into rare infectious diseases and associated hospitalizations during periods of heightened public health interest. Continued monitoring of hantavirus diagnoses and outcomes may help contextualize emerging outbreaks and support future research into the burden of severe disease.
These are preliminary research findings and not peer reviewed. Data are constantly changing and updating. These findings are consistent with data accessed on May 11, 2026.
Citations
- W. Muranyi, U. Bahr, M. Zeier, F. J. van der Woude, Hantavirus infection. Journal of the American Society of Nephrology 16, 3669–3679 (2005).
- V. P. Martínez, N. Di Paola, D. O. Alonso, U. Pérez-Sautu, C. M. Bellomo, A. A. Iglesias, R. M. Coelho, B. López, N. Periolo, P. A. Larson, E. R. Nagle, J. A. Chitty, C. B. Pratt, J. Díaz, D. Cisterna, J. Campos, H. Sharma, B. Dighero-Kemp, E. Biondo, L. Lewis, C. Anselmo, C. P. Olivera, F. Pontoriero, E. Lavarra, J. H. Kuhn, T. Strella, A. Edelstein, M. I. Burgos, M. Kaler, A. Rubinstein, J. R. Kugelman, M. Sanchez-Lockhart, C. Perandones, G. Palacios, “Super-Spreaders” and Person-to-Person Transmission of Andes Virus in Argentina. N Engl J Med 383, 2230–2241 (2020).
- J. N. Mills, J. M. Johnson, T. G. Ksiazek, B. A. Ellis, P. E. Rollin, T. L. Yates, M. O. Mann, M. R. Johnson, M. L. Campbell, J. Miyashiro, M. Patrick, M. Zyzak, D. Lavender, M. G. Novak, K. Schmidt, C. J. Peters, J. E. Childs, A survey of hantavirus antibody in small-mammal populations in selected United States National Parks. Am J Trop Med Hyg 58, 525–532 (1998).
- S. Singh, A. Numan, D. Sharma, R. Shukla, A. Alexander, G. K. Jain, F. J. Ahmad, P. Kesharwani, Epidemiology, virology and clinical aspects of hantavirus infections: an overview. International Journal of Environmental Health Research 32, 1815–1826 (2022).
- A. Vaheri, H. Henttonen, L. Voutilainen, J. Mustonen, T. Sironen, O. Vapalahti, Hantavirus infections in Europe and their impact on public health. Reviews in Medical Virology 23, 35–49 (2013).
- C. B. Jonsson, L. T. M. Figueiredo, O. Vapalahti, A Global Perspective on Hantavirus Ecology, Epidemiology, and Disease. Clin Microbiol Rev 23, 412–441 (2010).
- K. Dheerasekara, S. Sumathipala, R. Muthugala, Hantavirus Infections—Treatment and Prevention. Curr Treat Options Infect Dis 12, 410–421 (2020).
- CDC, Hantavirus Outbreak Toolkit, Hantavirus (2026). https://www.cdc.gov/hantavirus/toolkit/index.html.
- Hantavirus cruise: 17 Americans arrive in Nebraska for evaluation | CNN. https://www.cnn.com/2026/05/10/us/hantavirus-cruise-passengers-nebraska-facility.
- P. A. Vial, M. Ferrés, C. Vial, J. Klingström, C. Ahlm, R. López, N. Le Corre, G. J. Mertz, Hantavirus in humans: a review of clinical aspects and management. The Lancet Infectious Diseases 23, e371–e382 (2023).
- P. Makary, M. Kanerva, J. Ollgren, M. J. Virtanen, O. Vapalahti, O. Lyytikäinen, Disease burden of Puumala virus infections, 1995–2008. Epidemiology & Infection 138, 1484–1492 (2010).



