Schizophrenia treatment is rarely linear. Patients may discontinue therapy, add a medication, need escalating care, or cycle through periods of instability that carry real clinical and economic consequences. In a systematic review of US real-world oral antipsychotic studies, adherence was often below 50%, switching affected up to 50% of patients, and nearly a third required an additional medication. Higher total medical costs were associated with low adherence and treatment changes.
Those realities raise the bar for real-world schizophrenia research. To study the condition effectively, researchers need a complete, timely, representative view of the patient journey, including the ability to understand how treatment changes over time, capture the clinical context documented in notes, and study the social drivers that can shape access, continuity, and outcomes.
A real-world view of schizophrenia care
Schizophrenia is difficult to study through a single care setting or structured fields. Useful research depends on seeing medications, encounters, comorbidities, labs, clinical context, and social drivers of health together over time. Truveta Data was built to provide that view, with daily refreshed EHR data for more than 130 million patients—including clinical notes and imaging—linked with closed claims, mortality, and social drivers of health to support longitudinal research across the full patient journey.
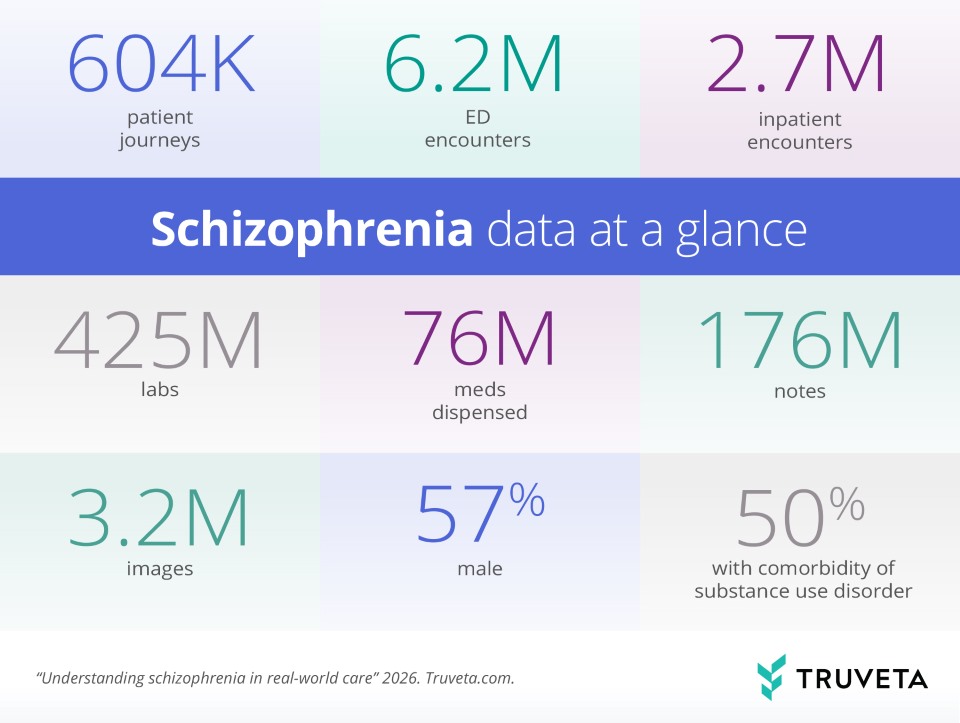
Where schizophrenia appears in acute care
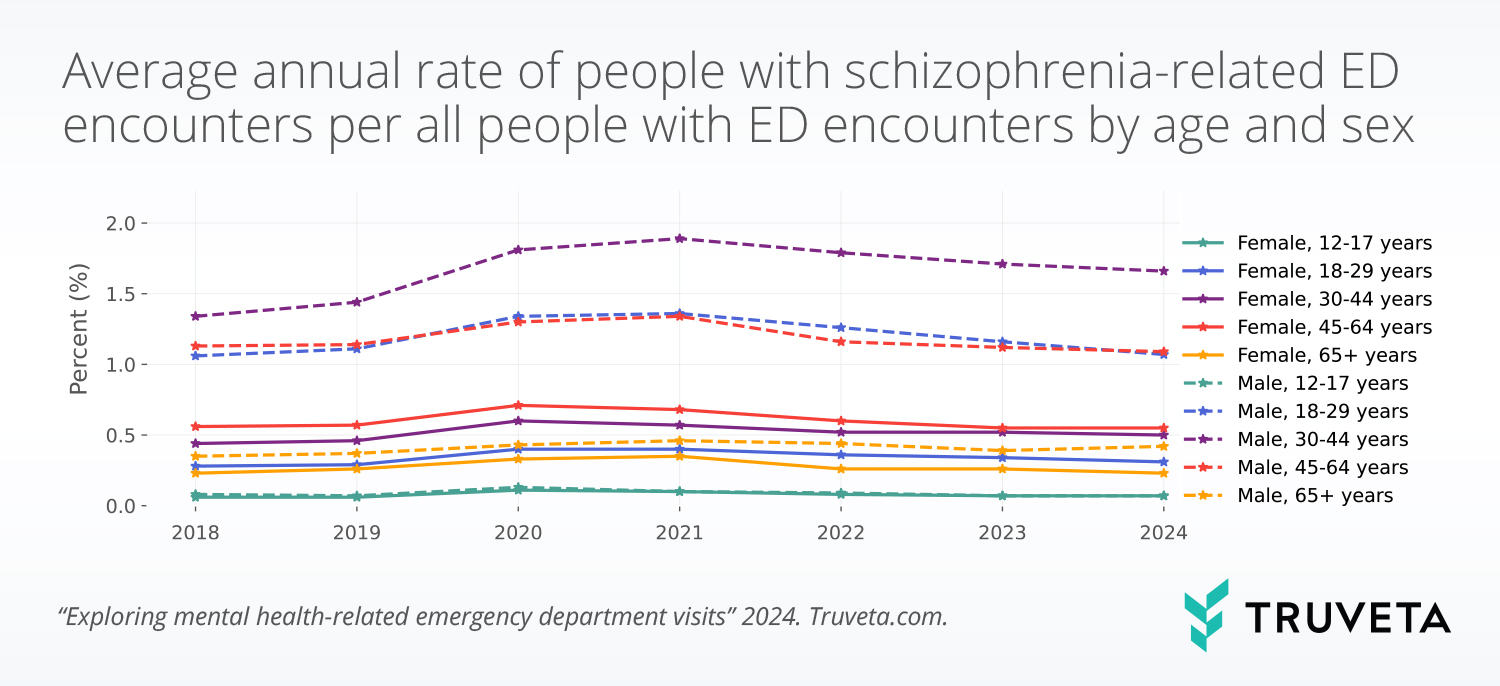
As emergency departments (EDs) manage a steady rise in visits related to mental health conditions, ED utilization offers a useful view of schizophrenia-related burden in practice. A recent Truveta Research analysis examined mental health-related ED encounters between 2018 and 2024 and found that schizophrenia-related visits followed a different pattern from several other mental health conditions, peaking in 2020 or 2021 across age and sex groups, and remaining elevated relative to pre-pandemic levels. Across the study period, males had roughly 2.5-fold higher rates of schizophrenia-related ED encounters than females, with males ages 30–44 showing the highest rates of any age and sex group.
These findings highlight where schizophrenia appears in acute care and which populations carry more of that burden. Researchers can help identify high-burden subgroups, frame questions about instability and care access, and place treatment patterns in the broader context of real-world utilization.
Prescribing patterns: Stable trends, meaningful differences
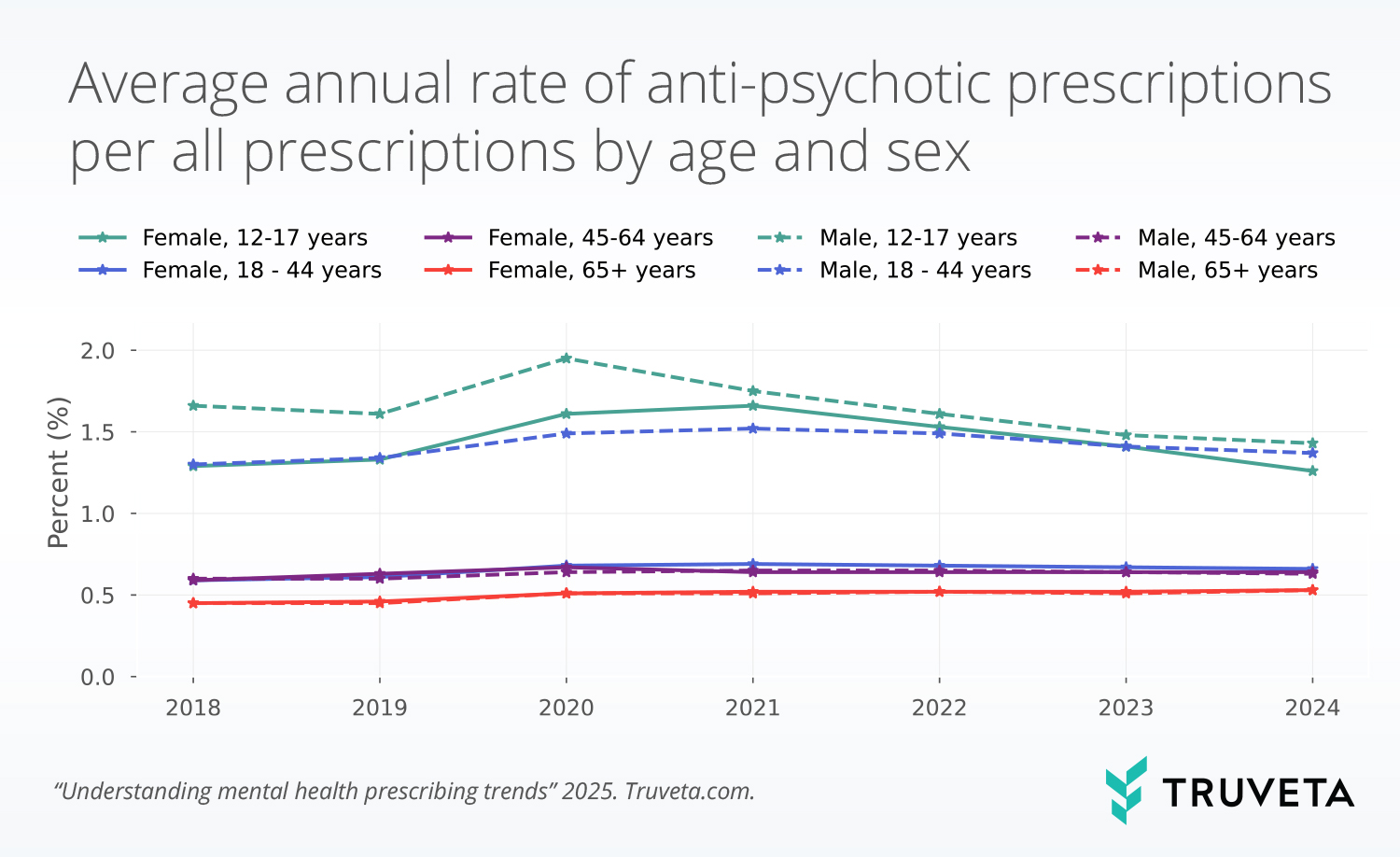
Treatment exposure is another important part of the schizophrenia story. In a separate Truveta Research analysis of mental health prescribing trends from 2018 to 2024, antipsychotic prescribing rates remained relatively stable overall, with modest peaks around 2020–2022 and higher rates among males and younger populations.
Those findings help ground schizophrenia research in real-world treatment patterns. They show that antipsychotic use is not evenly distributed across populations and that younger males account for some of the highest prescribing rates—a pattern consistent with the age and sex differences seen in schizophrenia-related emergency department use. Together, these results help frame where treatment burden appears in practice and why continued research into prescribing trends remains important as new therapies emerge.
Comorbidity burden of schizophrenia
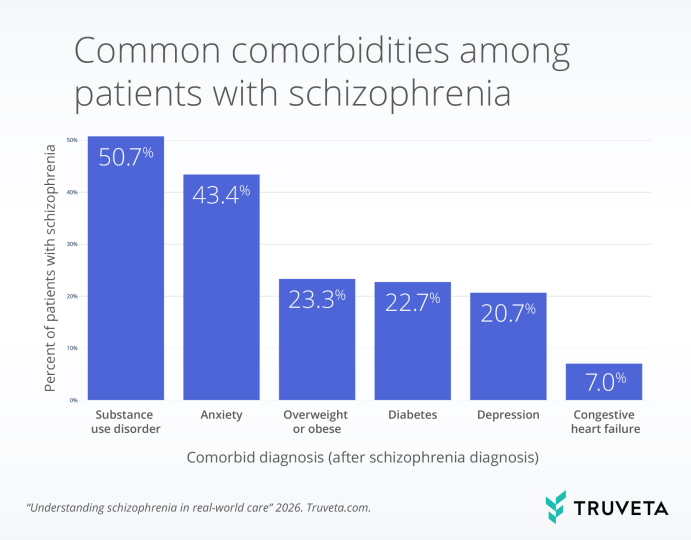
Schizophrenia is often accompanied by other conditions that shape treatment, utilization, and outcomes. In this cohort, anxiety, substance use disorder, obesity, and depression are among the most common co-occurring conditions.
That burden matters. Co-occurring mental and physical health conditions can influence treatment decisions, acute care use, safety, and long-term outcomes. The NIMH notes that approximately half of individuals with schizophrenia have co-occurring mental or behavioral health disorders, and that co-occurring medical conditions contribute to the elevated premature mortality seen in this population.
These overlapping conditions are often central to life sciences research, whether the goal is to understand unmet need, evaluate treatment patterns, study risk, or identify which patient populations may benefit most from new approaches to care.
Beyond structured data
In schizophrenia, important details such as symptom burden, functional decline, clinician rationale, and the context around treatment changes are documented in notes rather than coded data.
That context can meaningfully change what researchers are able to study. In a 2024 real-world analysis, predominant negative symptoms in schizophrenia were identified using natural language processing applied to semi-structured free text. Patients with those symptoms had greater psychiatric comorbidity, fewer days with an antipsychotic prescription, and higher rates and costs of psychiatric hospitalization.
This is an important area of differentiation for Truveta Data, which includes approximately 176 million clinical notes within the schizophrenia patient population. By linking structured data with concepts extracted from notes at scale, researchers can study treatment sequences over time, better understand the clinical context behind medication changes, and examine burden that would be difficult to capture from structured data alone.
Explore what’s possible
To explore how Truveta Data can support your schizophrenia research priorities, connect with our team for a custom feasibility assessment.

