The COVID-19 pandemic affected every aspect of many of our lives. For some, it affected how we work, where we work, who we interact with, and the frequency at which we interact with others. As we thought about the various impacts of social distancing, we were curious if periods of high COVID-19 case rates correlated with decreases in 1) sexually transmitted infections (STIs) and 2) birth rates 9 months later.
What we found was that in some cases, there appears to be a decrease in STI and conception rates at time points with COVID-19 peaks, especially later in the pandemic. However, because we didn’t account for seasonality of conception rates or factors which affect STIs, such as weekdays vs. weekends, there’s more to study.
Read on to learn more about the data we used, details on results, and the graphs of raw data by state.
Methods
Using a subset of the Truveta data set we looked at COVID-19 case rates, STI diagnosis rates, and conception rates (roughly 9 months before birth) across five states (California, Michigan, Ohio, Oregon, and Washington) between January 1, 2020 and March 15, 2022.
COVID-19 case rates
COVID-19 case rates were defined as a positive COVID-19 diagnosis or lab [1]. Patients were only included once. Daily COVID-19 case counts were calculated independent of vaccination status.
STI rates
We defined nine common STIs (Chlamydia, Gonorrhea, Syphilis, Mycoplasma Genitalium, Trichomoniasis, Herpes, , Chancroid, Granuloma Inguinale). We also included ICD10 diagnostic codes related to ‘Other predominantly sexually transmitted diseases, not elsewhere classified’ and ‘Unspecified sexually transmitted disease’. For each patient and STI type, only one occurrence was counted. We calculated the daily sum across the STIs to get a cumulative STI rate.
Conception rates
We estimated daily conception rates by looking nine months before the presence of a diagnostic code indicating a birth (ICD10 Z.38). We only included conception data June 15, 2021, as nine months of data are needed to see any trends.
Results
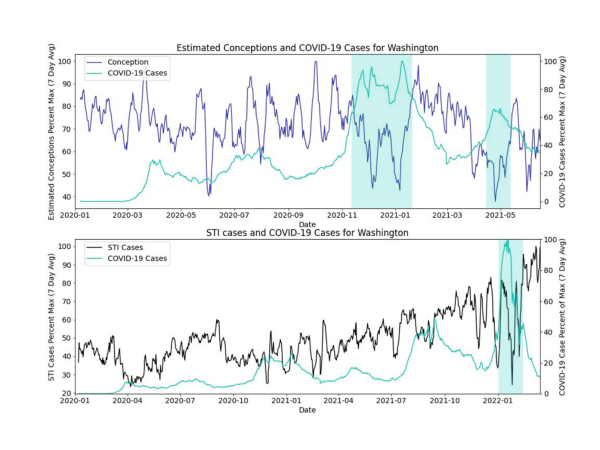
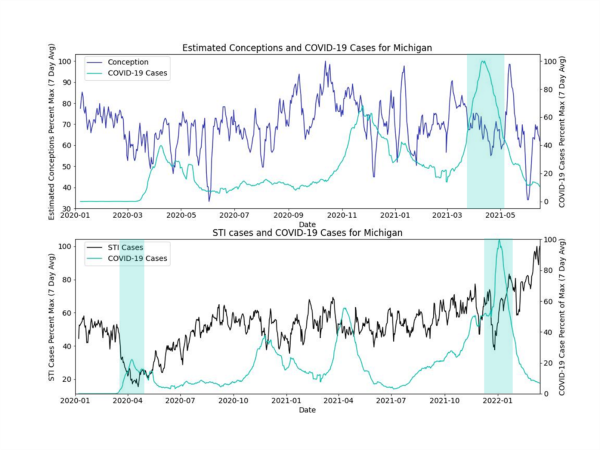
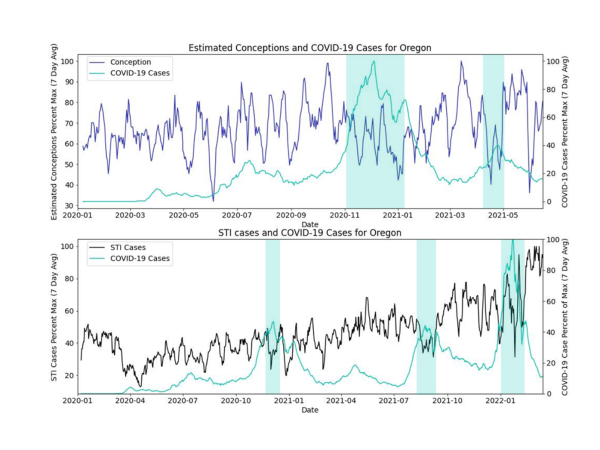
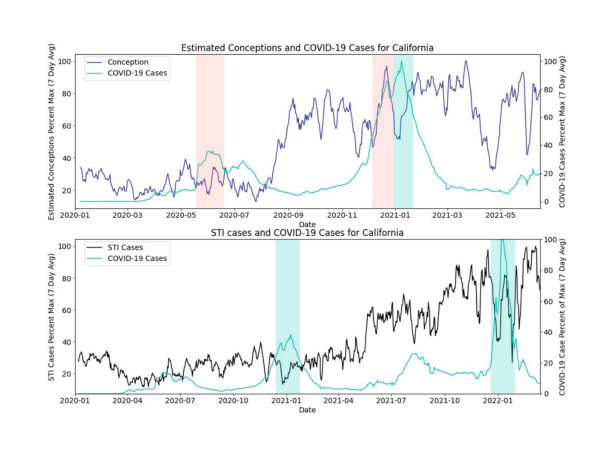
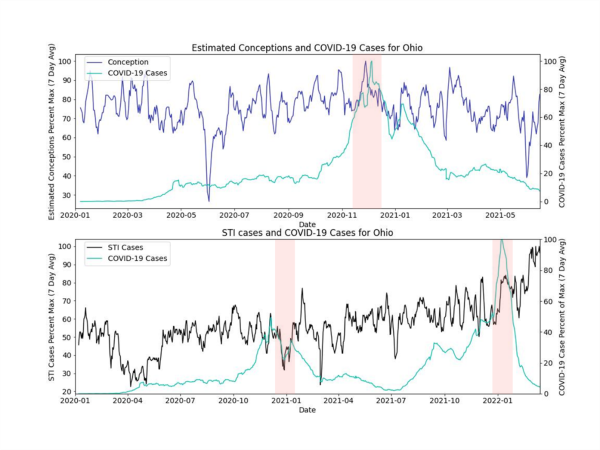
The figures below show the percent maximum of the 7-day rolling averages of COVID-19 rates, conception rates and STI rates. In these raw data, there may be correlations between increased COVID-19 rates and decreased STI and conception rates, especially later in the pandemic. We visually see periods with COVID-19 peaks that also correspond with decreased STI or conception rates, denoted in the figures with a green background. In these data we also see periods of high and low STI and conception rates that do not align with COVID-19 rates, denoted in the figures below with a red background.
There are likely many other factors at play that affect the numbers we have plotted (e.g., seasonal variability in births, lockdowns and masking restrictions in states, weekdays vs. weekends, full term/pre-term births, etc.). The variation in trends within and across states highlights the need to dig deeper into these data. The periods we’ve highlighted were chosen to represent the trends we visually see in these data and highlight a hypothesis.
These research methods and results should not be used to draw connections between fertility or STI rates and the COVID-19 virus. Rather, these raw data aim to show potential links between social outcomes of conception and STI rates correlated with COVID-19 rates.
Citations
[1] Smits, Peter D., et al. “Risk of COVID-19 breakthrough infection and hospitalization in individuals with comorbidities.” medRxiv (2022).doi: https://doi.org/10.1101/2022.04.26.22271727.
These are preliminary research findings and not peer reviewed. Data are constantly changing and updating. These findings are consistent with data from May 23, 2022.
