Older adults remain at highest risk for COVID-19–related hospitalization. Yet a new CDC analysis suggests that effective antiviral treatments are likely underprescribed among outpatients aged 65 or older, with prescribing patterns varying alongside disease transmission intensity
These findings were published in the CDC’s Morbidity and Mortality Weekly Report (MMWR), the agency’s primary vehicle for timely, authoritative public health information.
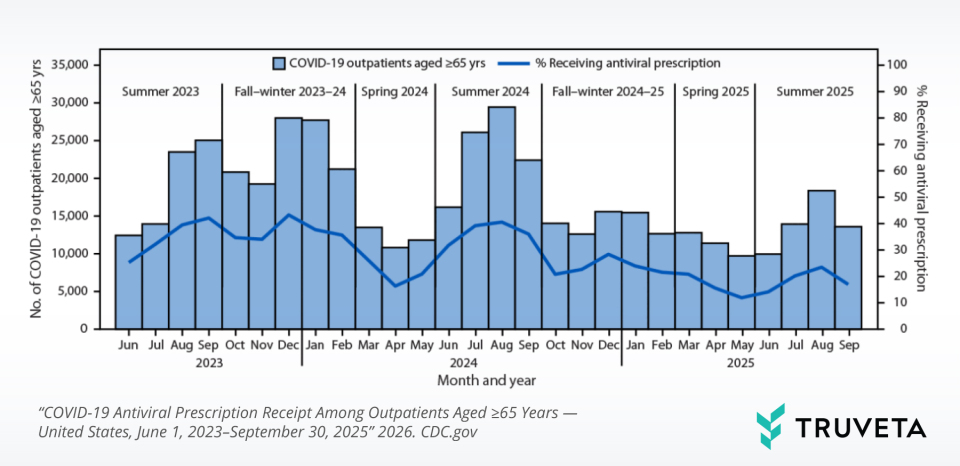
In the report, “COVID-19 Antiviral Prescription Receipt Among Outpatients Aged ≥65 Years — United States, June 1, 2023–September 30, 2025,” CDC researchers analyzed 482,456 outpatient encounters nationwide . The study used real-time, de-identified electronic health record (EHR) data from Truveta to evaluate how frequently antivirals were prescribed to older adults with COVID-19 and which factors were associated with treatment receipt.
What the CDC found
Only 16%–23% of adults aged 65 or older with a positive COVID-19 diagnosis received a COVID-19 antiviral prescription during certain periods of lower COVID-19 incidence, compared with 37%–38% during higher-incidence periods.
The analysis also identified meaningful variation across age groups, vaccination status, comorbidities, and rural versus urban communities. Notably, patients with comorbidities—who are at increased risk for severe disease—had lower odds of receiving an antiviral prescription.
Implications for public health
At a national scale, these findings reveal a critical gap in care for one of the highest-risk populations and highlight opportunities to improve treatment uptake among older adults.
The CDC concludes that antivirals are likely underprescribed among adults aged ≥65 and that increased prescribing, alongside continued vaccination, could reduce the risk of severe illness and hospitalization in this population.
Importantly, individual risk for progression to severe disease does not disappear when community transmission declines. The report emphasizes that both vaccination and timely outpatient treatment remain essential interventions for older adults year-round.
By examining prescribing patterns across seasons and populations, this analysis helps clarify where targeted education, awareness, and access efforts may have the greatest impact.


